From the moment Cristina, 30, saw the double lines form on her test in the spring of 2022, she knew she wanted to end her pregnancy. She was juggling grad school as well as two jobs—she couldn’t add raising a child on top of all of that. “There wasn’t a question at any point,” says Cristina, whose name has been changed to protect her privacy. The problem: She lived in Texas, a state perennially hostile to reproductive rights.
At the time, Roe v. Wade was still hanging on by a thread, but Texas’s notorious Senate Bill 8 was in effect, banning abortion past six weeks of pregnancy. Told she was too far along to receive care at a clinic, Cristina began researching online abortion pill providers but found that the drugs would take weeks to arrive and be cost-prohibitive. “At the time, I was constantly tired, constantly nauseous, and I just couldn’t get my workload done,” Cristina explains. “Another two weeks of that was just not feasible for me.”
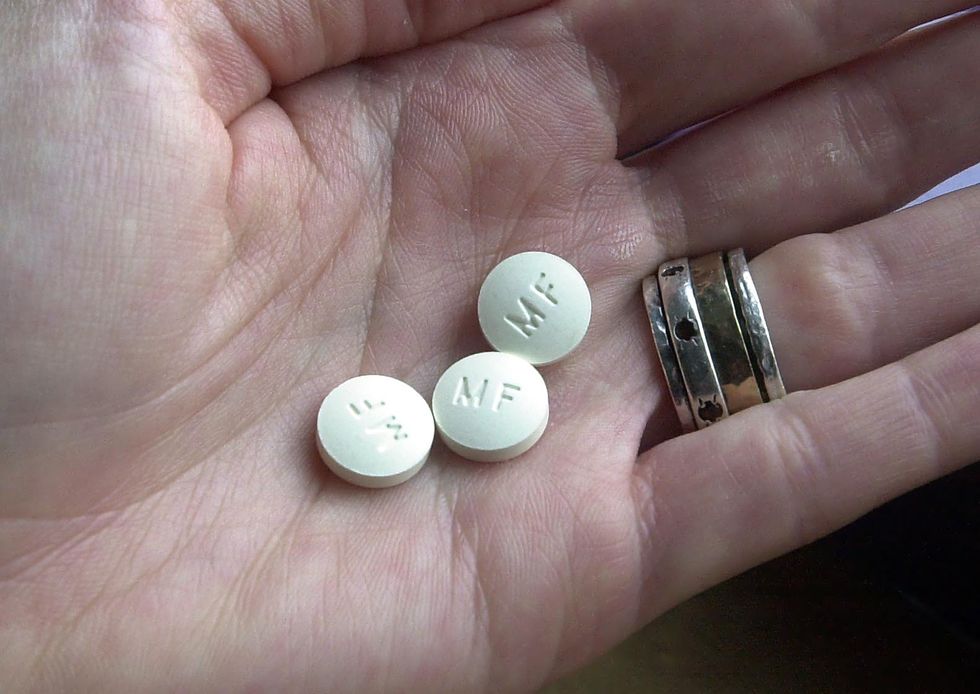
Finally, Cristina was able to get her hands on misoprostol—one of two safe and effective abortion pills that have been used to end pregnancies around the world for decades. Cristina received the medication in a brown bag without instructions and found a video posted by Doctors Without Borders on how to have a misoprostol-only abortion, but she was on her own to make sure she was doing it right.
After she took the pills, she experienced intense cramping and bleeding. “From what I knew, it had been a successful abortion,” says Cristina. But she had no way to know for sure that the medication had worked and was too afraid to see a doctor. About two weeks later, she noticed her nausea and fatigue begin to return and became anxious that she was still pregnant. She felt isolated, scared, and unsure of her next step, and she desperately wanted to talk to a doctor. Then she remembered: There was a number she could call.
Enter: the Miscarriage and Abortion Hotline, a free and completely anonymous helpline staffed by an army of volunteer health care professionals who provide confidential information to people across the country self-managing their abortions or experiencing pregnancy loss. The hotline is part of a growing and crucial network of virtual resources—such as online abortion pill providers, abortion funds, text lines for legal and emotional support, and a remarkably helpful subreddit—working to fill the health care void that existed even before the Dobbs decision overturned Roe. The toll-free service—currently the only hotline of its kind in the U.S.—is a lifeline for folks stuck in abortion-restricted states who are in need of support.
“I called the hotline, and they helped me determine that it was time to seek follow-up care, because all the signs were pointing to the fact that I might still be pregnant,” says Cristina. Despite her anxieties about documenting her pregnancy, she ultimately went to a local Planned Parenthood, which confirmed her fears: She was now about 9 weeks along.
Fortunately for Cristina, within hours, she was able to procure the mifepristone-misoprostol abortion medication regimen, which has been shown to be effective 96 percent of the time. (Cristina thinks the first time around, she may have taken an insufficient dosage or misunderstood the directions for misoprostol, which has an 88 percent effectiveness rate.) With the help of volunteers at the hotline who she called periodically through a second round of intense cramping, she successfully terminated her pregnancy. “They were the only medical provider that I could be 100 percent honest with about what was going on,” says Cristina.
Cristina is among a growing number of people who, faced with impossible restrictions, have sought to “self-manage” their abortions at home. Although definitions can vary, self-managing an abortion typically involves sourcing and administering pills on your own, outside the official supervision of a clinic or doctor. Self-managed abortions are different from telehealth medication abortions, where a clinician prescribes medication and walks a patient through the process virtually. Even before our current reproductive dystopia, a considerable number of American women—about 7 percent, according to one 2020 study—self-managed abortions at some point in their lives. With the end of Roe, some experts are anticipating that the number will rise further.
For Cristina, self-managing her abortion felt like the only option. “I am a visibly brown, Latina in South Texas,” Cristina says. “Among the list of people who may be questioned about what’s happening with their pregnancy, I’m pretty high up there.”
Increasingly, millions of people like Cristina find themselves staring down a yawning health care abyss when navigating complicated and extremely personal family-planning decisions. And while the DIY approach is essential in the era we live in, an abyss is still an abyss. That means that too often, folks are left to rely on internet searches and health-care-by-hotline to piece together medical care when they need it the most.
It’s exactly this gap that volunteers at the Miscarriage and Abortion Hotline say they’re trying to fill. People who call or text the toll-free number, 833-246-2632, anonymously connect with volunteer ob-gyns, family physicians, and midwives who serve as guides as they induce their abortions at home—the most common scenario the hotline handles—or in some instances, experience a miscarriage.
Sarah Stumbar, MD, a Florida-based family-medicine physician, says hotline volunteers like her field all kinds of questions from callers, who can speak to a doctor over the phone or via text. They ask, “Am I bleeding too much or too little?” and “I took a pregnancy test and it’s still positive—am I still pregnant?” and even “Can I eat while I take these pills?” (“Please don’t starve yourself!” says Dr. Stumbar.)
The hotline was founded in 2019 by a group of family-medicine practitioners in response to state-level barriers emerging during the Trump years. Since then, the network of volunteers and the volume of calls has grown exponentially. “We’ve increased in size twice since Dobbs,” explains founder Linda Prine, MD, a family-medicine physician in New York. “When you’re on, you don’t move from your seat. You’re answering calls and texts nonstop.”
Today, a group of about 70 providers volunteer for 6-hour shifts and handle anywhere between 50 to 70 calls a day, answered between 8 a.m. to 2 a.m. ET. The clinicians are all experienced in abortion care and miscarriage management and receive additional resources on local abortion laws so they understand the nuances of each caller’s situation. Dr. Stumbar says calls come in at all hours of the day, from all corners of the country. “We close for just a few hours, but there are always calls that come in between 2 a.m. and 6 a.m.,” says Dr. Stumbar. “I just envision people at home all alone with no one. And they’re reaching out to a stranger over the phone. It makes me feel very lonely for them.”
Hotline volunteers say that they want to ensure that those going through what can be a stressful and vulnerable experience don’t have to do it all alone. April Lockley, DO, a family-medicine physician based in New York who serves as the medical director of the hotline, says callers often just want a little reassurance. “They want to double-check that they’re reading the instructions correctly, that the side effects they’re experiencing are normal, or they’re wondering how they’ll know if the process worked,” she explains.
In the last year, hotline volunteers say they’ve noticed a change in the tenor of the calls. “These days, people are stressed beyond belief,” Dr. Prine says.
“I was talking to someone from Texas recently who’d had a miscarriage, but she was too scared to go into the doctor because she was afraid that they would think she took pills,” says Dr. Stumbar, “And she was so grateful to have found someone she could talk to because that fear was just so prevalent—even though she’d literally done nothing.”
When callers are concerned about their legal liability, hotline volunteers often refer them to the Repro Legal Helpline, a legal aid group that helps people understand their rights in abortion-restricted states.
For Cristina, her abortion was more harrowing than she expected. “It was pain to a level that I had not prepared for,” she says. “My cramping continued for over 5 hours, and I was very much concerned about possibly having to go to the emergency room. Luckily, I was again able to contact the Miscarriage and Abortion Hotline and they basically let me know that if the cramping went past 6 hours, that it might be a good idea to go to an emergency room.”
Dr. Prine says it’s rare for a hotline volunteer to recommend that a caller go to the hospital, like they considered with Cristina. They try to avoid it because complications are rare and they want callers to be able to avoid the stress and expense. “We have a rule on the hotline that if we are thinking of sending somebody to the hospital, we consult with each other first to make sure it really, really seems necessary because we don’t want people to get in trouble,” explains Dr. Prine.
But in those uncommon cases where they do think a visit to a hospital is necessary, Dr. Prine says they suggest that callers tell their doctors they’ve had a miscarriage. “There’s no way to tell if a person has self-induced their abortion or if they are just having a spontaneous miscarriage,” notes Dr. Prine. “So as long as the person doesn’t divulge they’ve taken pills, they can’t be charged with anything.”
At around the 5 hours and 45 minutes mark, Cristina’s cramping stopped. “I began bleeding. I was able to pass the pregnancy, and it was very evident at that point that I had had a successful abortion.”
Now a year later, as the courts consider the fate of mifepristone and abortion providers gird for the possibility of a miso-only protocol, Cristina says that she’s grateful she was able to end her unwanted pregnancy, although she knows not everyone has access to the same resources: a phone, stable internet, and a safe place where she could manage her symptoms in private. “It’s reassuring for me that even in the state of Texas, in conditions such as these, I was still able to exercise choice,” says Cristina, “but it’s also a Band-Aid that leaves a lot of people out.”
Even volunteers acknowledge that the hotline, while critical right now, can’t close an ever-widening access gap on its own. But it’s the push to fill that void that drives Dr. Stumbar to continue her work. “I just love speaking to people on the hotline. You hear so many different accents, women from so many different places, and it makes you feel really connected,” she says, “like a part of a bigger community that I wish we didn’t need to have.”

Sara Hutchinson is a freelance journalist covering public health and public education in a post-Roe America. Her writing has appeared in The Washington Post, The Hechinger Report, The Texas Observer, and many others.